CATARACT
WHAT İS CATARACT?
 Cataract is an eye disease which starts with clouding of the lens and cause significant reduction in vision. It is 90 % age-related, however a secondary cataract might occur due to some traumatic diseases, uveitis, use of some medication like steroids. Age-related cataract may also develop in both eyes although it is usually asymmetric. Blurry vision, low quality in color vision, gradual reduction in visual acuity are the most common symptoms of cataract.
Cataract is an eye disease which starts with clouding of the lens and cause significant reduction in vision. It is 90 % age-related, however a secondary cataract might occur due to some traumatic diseases, uveitis, use of some medication like steroids. Age-related cataract may also develop in both eyes although it is usually asymmetric. Blurry vision, low quality in color vision, gradual reduction in visual acuity are the most common symptoms of cataract.
It can be detected in early period by regular eye examinations and determined the time of the treatment. Therefore, a regular eye examination is necessary for the people over 40 years old.
CONGENİTAL CATARACTS
Congenital cataracts can also be watched in babies. Rubella or taking some antiviral medications in the early period of pregnancy lead the development of congenital cataract. Congenital cataract can only be observed by very careful families. A pediatrician always checks out the presence of congenital cataracts in general examination. Babies eyes should be examined every year. Early examinations at the age of 2 or 2,5, are very important to protect any upcoming amblyopia (known as Lazy Eye).

WHAT İS THE BEST TİME FOR SURGERY?
As the vision of the patient gets unsatisfactory and from the time of detection of cataract, surg ery can be performed. It is not a good behavior to wait for it to be developed and get harder. Because it can be more difficult and longer healing time if it is operated in the late stage of the disease.
ON THE DAY OF SURGERY
-You can have some light food before surgery. However, children mustn’t take any food or beverages 6 hours before operation if the operation is performed under general anesthesia due to some reasons.
-You shouldn’t take any medications for diabetics or asthma on the day of operation but, you should keep taking Insulin or oral antidiabetics and your diet.
– It is recommended that you should bring those systemic medication with you.
– Please leave your valuables at home.
– Face must be washed well and kept free of any make ups or perfumes.
– You will be asked to put on special surgery gowns.
– You will be asked to keep your eyes and head still for a short time during the operation
– You can go home on the same day just after a while. Your surgeon will call you for post-op examination within 36 hours.
– Its highly recommended that, you should not drive and go back home alone.

OPERATİON PERİOD
Cataract surgery takes about 10 to 15 min according to the cataract and experience of the surgeon.
RECOVERY PERİOD
It varies depending on the hardness of the cataract and surgeon’s experience to get normal vision back. Patients can usually have maximum visual ability at the end of a week or two. Full visual acuity will be reached between 15 and 30 days after operation. The recovery time could also be within a few days if treated just on time.
ARE THERE ANY RİSKS AFTER OPERATİON?
Every surgical intervention may have some risks like infection. Patients are given some antibiotic eye drops which must be used properly within first 48-72 hours against infection. Patients also must be very careful to keep your eyes as hygienic as possible.
Patients with Any sudden vision loss, severe pain or overproduction of rheum must see their surgeon immediately.
You must use spectacles for distant or near vision with the standard lenses implanted during the surgery. Even though with the use of spectacles, you may not be able to see intermediate distances as 75-100 cm.
Now, you can easily have very clear vision at all distances with the help of multifocal lenses if you don’t have any other discomfort except for cataract.
EYE CARE AFTER OPERATİON
- Do not rub your eye or give any pressures.
- Try not to sleep on your eye to protect it from pressure.
- Avoid washing your eye or hot tub for the first a few days. But you can wipe your face to clean.
- You could take a warm shower protecting your eye from water.
- It is not a good idea to swim for a while until you are allowed by your eye physician.
- It is normal to feel sensitivity to light, watery, sting or light redness in your eye
- You should put on sunglasses on windy or sunny days.
- You can keep on your daily activities such as reading, walking or watching T.V
- Blurry vision which will disappear following days is very normal.
- You can use your old spectacles after surgery. However you may not see well due to the change in your glasses prescription.
- Your new glasses would be given within 3-6 weeks after operation.
- Try to avoid bending over or heavy lifting for a while.
- Don’t drive unless you are allowed by your doctor.
- Make sure you use medications and visit your doctor on time.
LASER EYE TREATMENT
The world’s most widely used method of laser treatment is Lasik. After local anesthesia, a very thin flap under which laser lights are applied to correct the refractive errors is created and put back into its place. Patients feel no pain during 4-5-minute-long operation and can go back to their normal life the following day.
PRK
In this method, excimer laser pulses are sent to make corrections after removal of epithelium which is the outer layer of the cornea. Epithel tissue recovers by itself within 3 days.
LASEK
In this method, before application of laser correction under epithelium, epithelium is weakened by an alcoholic solution and folded back. Excimer Laser pulses make the necessary corrections, and the epithelium flap is placed back. Recovery time is within 3 days.
LASIK
A very thin flap is created by a microkeratome and folded back. Excimer Laser corrections are made on the tissue underneath then the flap is placed back.
I-LASIK – FEMTOSECOND LASER
This is a combination of both Intralase lazer technology and Customized Excimer laser.
WHICH METHOD SHOULD I PREFER?
Intralase laser technology, I-Lasik is the worlds most preferred and comfortable treatment method. Hovewer for some cases which the eyes are not found suitable for I-Lasik, Lasek or PRK (Ablation on the outer surface of the eye) could be applied. The only disadvantage of those techniques is a little longer recovery time.
IS LASER TREATMENT SAFE?
Excimer laser treatment has been started after years of clinical studies and medical knowledge. It is also approved by Food and Drug Administration in the USA.
COULD IT BE APPLIED AGAIN?
- This actually depends on the thickness of the cornea.
- In case of recurrence and suitable cornea thickness, it can be applied again.
- Only 5 % of the cases may require another application.
- It may occur again if the correction has been applied on the eyes with high dioptrics or overreacted eyes.
- Since mikrokeratom will not be used again, a secondary laser treatment will be more comfortable for the patient.
LASIK PROCEDURE
- STEP 1 – WAVEFRONT TEST
The first step is to measure your eyes’ unique characteristics by wavescan technology. WaveScan technology is used to get 3D map of your refractive errors. Each eye has unique characteristics which are different even from each other. Therefore, every laser treatment should be planned according to these specifications to receive the most successful results. Afterwards, Advanced Custom Vue program designs your customized treatment accordingly.
By this technology, laser pulses are easily be programmed counting any tiny details about your eye during laser treatment.
- STEP 2 – FLEP CREATION
In this method, Full Computerized IntraLase technology is used to create a very tiny flip on our cornea by sending laser pulses without using of a blade.
- STEP 3 – CUSTOMIZED LASER CORRECTION
Until now, all detaied analyses have been carried out by wavescan and a unique flip has been created by Intralase technology. Advanced custom Vue technology which has been the only FDA approved laser method corrects myopia, hyperopia or astigmatism perfectly. Any minimal movement of the eyes are tracked instantly and corrected without any errors by this Autofocus technology developed by NASA.
WHY LASIK?
- It takes only 15-25 seconds for laser application and appx. 10 minutes for the total treatment.
- It is the worlds most preferred laser technology
- It is not necessary to cover the eye or keep the patient in the hospital.
- Both eyes can also be treated at once if necessary.
- Visual aquity can be corrected in the same session.
- This is a very secure treatment to make any necessary corrections related to myopia, hypermopia and astigmatism.
- Since the results will never be changed after 3 months, It is a long-lasting treatment.
- As it is applied directly on the cornea, no significant marks can be seen from the outside.
- It has been completely safe treatment of which the success depends on the surgeon’s experience and the technology used.
- After operation, your glass dependancy disappears and more comfortable life will start. Your new prescription either will show no or a tiny change after 3 months.
SUPERIORITIES OF LASIK OPERATION
- Lasik treatment corrects myopia at all levels.
- Recurrence is not expected for low eye measures.
- Your eye measures will be consistent within a short time.
- It can be applied to both eyes at once.
- Hospitalization is not necessary.
- Patients may go back to normal life within 24 hours.
- In-build Turbo Eye Tracker is a unique system which tracks all the vertical and horizontal movements on the patient’s eyes.
- Any tiny difference between horizantal and vertical position of the patient is automatically adjusted and corrected by the Static Torsion Management System.
- All rotative movements are also controlled and corrected by the Dynamic Torsion system.
WHO CAN HAVE THIS TREATMENT?
- People over 18 who have been using glasses or lenses permanently
- People who don’t have eye disease like keratoconus or Glocoma
- People who don’t have any systematic disease like diabetis or rheumatism.
- People who have permament eye prescpription for a year min.
- Women who are either not in pregnancy or brestfeeding period.
THINGS TO BE REMEMBERED BEFOREHAND
People who have been using rigid contact lenses must quit using them 3 weeks prior to the surgery. People who have been using soft contact lenses must quit using them 1 week prior to the surgery. You have been given all the fundamentals of lasik treatment. Now you can make your last step which is to get an appointment from your eye surgeon to find out the best available treatment for your eyes’ refractive errors.
KERATOCONUS
CORNEA
Cornea is the outer layer of our eyes that protects our natural lens and give us a clear vision by determining the refraction of the light.
 It is a progressive disorder that the round-shape cornea gets thinner and bulges out into the shape of a cone. Then this cone-shaped cornea causes distorted vision and irregular astigmatism. It normally affects both eyes.
It is a progressive disorder that the round-shape cornea gets thinner and bulges out into the shape of a cone. Then this cone-shaped cornea causes distorted vision and irregular astigmatism. It normally affects both eyes.
CAUSES OF KERATOCONUS
- It occurs especially in teens.
- Genetic predisposition (ıf any member of the family has it)
- Rubbing the eye steadily due to allergic conjunktivitis.
- Central contact of the contact lenses.
- A habit of sleeping face down with some pressure to the eye for a long time.


DIAGNOSES
A developed keratoconus can be diagnosed very easily in a normal eye exam. But it can only be diagnosed in more complex examinations if it is at early stage. So it might not be observed in a normal eye exam. In addition to them, If glass prescriptions change quite often, If visual acuity is less than 10/10 despite glass use, In case of genetic predisposition in the family Further examination techniques are required.
TREATMENT
 The way of treatment in this disease firstly depends on your eye specialist who has been evaluating the progress. The success of the treatment depends on the experience and excellency of your eye doctor, stage of keratoconus, developed technology beside the quality of the equipments and products used in your treatment.
The way of treatment in this disease firstly depends on your eye specialist who has been evaluating the progress. The success of the treatment depends on the experience and excellency of your eye doctor, stage of keratoconus, developed technology beside the quality of the equipments and products used in your treatment.
GLASSES
They could be used at early stages beside every stage of the treatment. They only give a better vision but may not stop the progression of keratoconus. In case of progression, the vision may not be corrected due to irregular astigmatism which can require new glass prescriptions that causes the patients discomfort.
CONTACT LENSES
People who do not want to wear glasses or benefit from them, can wear soft contact lenses at early stage of keratoconus. At late stages, semi-rigid and gas permeable contact lenses could be used. Although the purpose of contact lenses is to give a better vision, they might not be tolerated by your eye. Not only do they help stop the progression of keratoconus, but also, they might cause some irritation on the cornea due to the lack of lubrication between the cornea and the lenses.
INTRACORNEAL RINGS
It is applied to the people whose cornea thickness are found to be suitable for this operation. This operation is performed with topical anesthetic drop-in operation room. Two tiny crescent-shaped pieces are inserted into the center of the cornea during this operation. The purpose of this operation is to correct the misshapen cornea as much as possible. Rings are tolerated by the eye perfectly. Although it is a very beneficial treatment, it still may not stop the progression of keratoconus. But people have reported that they have much better vision after this treatment.
CROSS-LINKING
It is very reliable method which is applied to the patients with progressing keratoconus. The thickness of the cornea is very important in this process. After numbing the eye with topical anesthetic drops, Vitamin B2 (Riboflavin) is dropped on the cornea under UVA lights for about 5 minutes. This process strengthens collagen tissue of the cornea and may ease or stop the progression. Patiens can go back to their normal life just a few weeks after the operation.
CORNEAL TRANSPLANTATION – KERATOPLASTY
Only 20 % of the keratoconus patients may need a keratoplasty operation. These are the cases in which all other treatments could not stop the progression. In this surgical intervention, a round-shaped tissue which is appx. 7 mm in diameter is removed and changed with a healthy tissue which is derived from a donor. This tiny tissue is replaced with stitches.
Even though the success rate is very high in this method, it can be the last to think in treatment due to the difficulty in finding a healthy tissue from a donor and long recovery period.
REMEMBER
- Early diagnosis and periodical exams are vitally important in this disease.
- Patients must be followed up by the surgeon after surgery.
- Patients can go back to their normal life just a few days after surgery.
- The first purpose of this surgery is to ease the progression of the disease.
- It has been observed great improvement and better quality in patients’ vision.
When cornea gets thinner and become pointed it is called Keratoconus. Cornea has curvy shape, and this is bolded by birth, and it increase so cornea hangs down. Increasing causes astigmatism. There are four types of level. First level is light, second level is mild, third level is heavy and forth is advance level of keratoconus. First symptom of keratoconus is flu vision. Sensitivity for light, glare, reduce night vision, headache, difficulty of reading, double vision, burn and feeling sting are other symptoms of keratoconus. It is effect patient’s life quality. Vision could be affected very badly. Keratoconus usually happens eye but sometimes one of them could be heavier. Rate is almost same for genders. It is usually notice on teen ages.
Doctors can be suspicious about patients who have astigmatism that increase every examination. If patients do not pay attention on that cornea could be dangerously thin. Permeable hard lenses uses on keratoconus because soft lens do not fix shape of cornea. Patients and doctors should be careful and patient for who are using permeable hard lens because usually patients who use this lens do not feel comfortable.
Corneas inside connection can be stronger with ultraviolet A and eye drop form riboflavin. This treatment is using to stop cornea to hang down. Internal corneal rings developed for patients who have keratoconus. Two half circle transparent rings placed inside of the cornea. They do not stop cornea to hang down but they fixed problem with vision temporarily.
Twenty percent of the keratoconus patients go to have corneal transportation operation. Corneal transportation is changing center to 7-9 mm of the cornea with new one. Usually patients go to have corneal transportation when they have late diagnosis for keratoconus. Success of this operation is ninety-five percent but sometimes it may cause serious complication.
GLAUCOMA
Glocoma (its known as eye pressure in common) is a serious eye disease for people over 40 mostly. It may develop gradually within years and damage optic nerve which allows gives us the ability to see. When vision loss occurs, it is impossible to take it back. So, early diagnose is very important for the prompt and available treatment. A detailed eye check which can only be done by developed technology could be performed at all Batıgoz and West Eye hospitals.
SYMPTOMS;
- Increased headaches mostly in the morning.
- Blurry vision at times
- Haloes around lights at night
- Pain around eyes while watching the T.V
INCREASING FACTORS OF GLAUCOMA
- Genetic predisposition of Glaucoma
- Being over 35 years old
- Diabetics
- Severe Anemeia or shocks
- High or Low Blood Pressure
- High Myopia
- High Hypermetropia
- Migrane
- Steroid taking for a long time
- Eye injuiries
- Racial Factors
People who have above are most likely to have the risk of glaucoma rather than other people. These people must visit their doctors regularly and often to diagnose the damage on their optic nerve.
DIAGNOSES
Developed diagnostic equipments are used to follow up the glaucoma and any possible damages on the optic nerve. These diagnoses are;
- OCT – Optical Coherence Tomography – Imaging of cross-sectional images of Retina
- HRT – Heidelberg Retina Tomography – Diagnose of the optical nerve damage
- PACHYMETRY – Measuring the thickness of cornea.
These three are very important to diagnose and plan the treatment of Glaucoma.
TREATMENT METHODS OF GLAUCOMA
- There are 3 ways to treat
- Medication
- Laser Treatment
- Surgical Treatment

Medication: There are different eye drops used in medication which reduce the pressure in the eyes. They are used regularly and permanently. If its seen unsatisfactory, second eye drop is added to the treatment. If the eye pressure is still not at normal level, the third drop may also be used according to the doctor’s decision. If it insists, another treatment is necessary.
Laser Treatment: It can be applied to the people who have no benefit from medications. This treatment is a very successful method if it is performed on time prior to the surgery. Two kinds of laser therapy are used which are.
ALT – Argon Laser Trabeculoplasty
A drainage channel is created by Argon Laser to drain excessive intraocular fluid in the eye.
SLT – Selective Laser Trabeculoplasty
If ALT is not satisfactory, then a drainage channel is created by lower-level selective laser.
Surgical Treatment: In this way, a drainage channel is created on the white part of our eye by surgical method. Thru this nearly invisible tunnel, intraocular fluid is drained to lower the pressure in the eye.
WHAT İS GLAUCOMA?
This is an insidious disease which may end up with visional loss if not diagnosed and treated on time. Therefore, annual examination is very necessary to diagnose it.
This term is used to explain a set of damages on the optic nerve. The only reason is caused by the high pressure in the eye.
When the normal circulation of our intraocular fluid (aquos ) is blocked partially or fully due to some reasons, eye pressure starts to increase. (It may also develop without it)

RELEX SMILE
RELEX SMILE is a custom and bladeless high tech laser surgery which is known as the 3. generation in laser vision correction. With this technique, myopia (up to -10) and astigmatism (up to -5) can be cured in our Istanbul and Izmir branches.
The Benefits of ReLEx SMILE:
- Applicable for thin corneas
- Applicable for high myopia and astigmatism
- Better protection of corneal structure
- Flapless operation with single step solution
- The nearest natural outcome
- Dry eye incidence is reduced.
ANGİOGRAPHY
WHAT İS ANGİOGRAPHY?
It is a technique for examining the circulation of the retina and choroid on the back of the eye.
WHY İT İS İMPORTANT?
It helps to diagnose of diabetes, eye tumors, night blindness and retinal disorders.
WHY İT İS DONE?
- To display the eye veins
- To investigate the presence of any mass within the eye
- To determine vascular leakage in the eye
- To investigate bleeding of blood vessels in the eye
- To determine a vascular congestion in the eye
- To examine the eye inflammation
- To determine the location for the laser treatment on the retina
- To confirm the effectiveness of the treatment
- To detect the age-related yellow spot disorders
HOW İT İS DONE?
Angiography is a technique for examining the blood vessels in the eye with using a special dye. It helps to see some unseen problems, to diagnose and choose the treatment for the patient. In the beginning, the patient’s pupils are enlarged with eye drops and an injection is made. After the medicine is reached to the eye within the circular system, the blood vessels can be seen more clearly. At this moment, by using a special microscope and a blue light, an angiogram is obtained by photographing the medicine. With this photograph, the patient is diagnosed. This usually takes 30 minutes and there is no harm to the patient’s eyes.
OPTİCAL COHERENCE TOMOGRAPHY (OCT)
The OCT is also known as a new generation of technology in unmedicated imaging.
The movement of the moving red blood cells within the vessels are captured with OCT-B screening and rendered as an image.
In OCT imaging angiography, vascular and structural information is displayed on a single screen without invasive intervention. As in traditional eye angiography, patient is not given medicine intravenously. 3D angiographic imaging of the eye is provided with this technique.
WHY ANGİOPLEX?
Retina and choroid layers can be examined separately for ease of visual assessment.
It is a non-invasive, drug-free angiography.
With only one scan, OCT angiography is provided.
OCT ANGİOGRAPHY
With 3D , the rear layers of the eye can be evaluated one by one.
It is a drug-free angiography.
With one scan, the procedure is complete in a short period of time.
The pupils are not enlarged with eye drops.
FLOATERS
Floaters : The treatment of filamentous and fuzzy objects in the vitreous
WHAT İS VİTREOLYSİS?
Vitreolysis also known as laser treatment for eye floaters is a painless procedure that can be applied to the outside of the eye to eliminate visual disturbance due to floaters.
The objective of this process is to perform a functional recovery.
In short, the purpose of the vitreolysis is to allow the patients to return to their normal daily activities
without fuzziness.
HOW VİTREOLYSİS WORKS?
Vitreolysis eliminates vitreous strands and particles which cause vitreous haze by evaporation with nanosecond laser beam shot. During this process, molecules of collagen and hyaluronic floaters is converted to a gas. As a result, the floaters are either removed or decreased to a minimum amount that will not affect your vision.
WHAT HAPPENS DURİNG THE PROCESS?
Vitriolizes is an outpatient procedure performed; There is no need to stay overnight in the hospital. Just before the treatment, the eye doctor will apply an eye drop which provides a mild anesthetic effect.
Then a special microscope will be used for applying laser beams to your eyes through a contact lens which is in contact with your eyes.
During the treatment, you will possibly see the floaters turning into gas bubbles and some small stains or shadows. These gas bubbles will dissolve and will be absorbed in vitreus.
After the treatment, your eye doctor can apply an anti-inflammatory eye drop to your eyes.
A single treatment session can be 20-30 minutes and most of the patients need 2 or 3 sessions to maintain a perfect treatment.
WHAT İS WAİTİNG FOR ME AFTER THE TREATMENT?
After the treatment, you may observe some small dark stains just under you view but these little gas bubbles will disappear in a short period of time. In some occasions, patients may feel a little dizzy or may encounter a blurred vision.
COMPLİCATİONS AND ADVERSE EFFECTS
There are so little side effects in the reports of vitriolizes and they can be a sudden increase of eye pressure or can be cataract.
WHO CAN BE TREATED?
Eye examination is necessary in order to understand your eligibility for vitreolysis treatment.
*Age : In patients whose ages are below 45, the vitreolysis treatment is not suggested due to the distance of these floaters with the retina is so near as 1-2 mm.
*Start of the symptoms : If the floaters are increased in short period of time, maybe there can be a correlation with PVD (Posterior Vitreous Detachment). Vitreolysis can be performed on this situation.
*Characteristics of floaters : Large floaters who are away from the retina’s soft borders are ideal for vitreolysis treatments.
WHAT İS DEGENERATİVE VİTREOUS SYNDROME ?
The vitreous body is the clear gel that fills the space between the lens and the retina of the eyeball of humans.
Vitreous fluid at a young age is completely transparent. When we get older, the vitreous fluid begins to lose its shape and starts liquefying. In this case of non-stable vitreous, collagen fibers collapse and they stick together to form clusters. These can be seen as dots, strands or webs because of they make shadows on retina. This is usually called as floaters.
In most of the cases, when the patient is old, vitreous can be detached from the retina. This is known as PVD (Posterior Vitreous Detachment). In PVD, the floaters increase suddenly.
TYPE OF FLOATERS:
Floaters are flying little particles in vitreous body. The shadow of these particles falls on retina, the light-sensitive layer of tissue behind the eye. If you have floaters, you may see these shadows flying on your view.
FİBROUS FLOATERS
As a result of collagen fibers are clustering in the vitreous, the thin, dense floaters occur and/or some form of spider webs can be seen. This is mostly seen on teenagers. These floaters can be treated by vitriolizes depending on the size and location of them.
COMMON FLOATERS
This cloud shaped floaters can be occurred due to the natural aging process. This kind of floaters can be cured in one session of vitriolizes, but on some occasions the patient may need a couple of more sessions to be perfectly cured.
WEİSS RİNG FLOATERS
This is usually a big floater far from the lens and the retina. So that the vitriolizes can be performed in an effective and secure way.
WHAT İF VİTREOLYSİS WON’T WORK FOR ME?
Clinical studies have shown that vitriolizes is a safe and effective treatment for most patients. If the floaters are visible again, the doctor may suggest a surgery.
There are different surgery types according to the diagnosis. In the operation, the vitreous can be changed with a stable salt solution. This operation has a risk of infection and bleeding. Also as a result, there can be a formation of cataract. This operation lasts for 1-2 hours approximately.
RETİNAL TEARS AND RETİNAL DETACHMENT
WHAT İS THE REASON OF RETİNAL TEARS AND HOLES?
 Retina has a contact with vitreous gel inside of the eye. Vitreous gel is homogeny, tight, support the retina and pushes outer tissues such as choroids and sclera in healthy eye. Vitreous gel’s viscose and homogeny structure may change in some special cases. High myopia, eye trauma and intraocular inflammation diseases may vitreous gel turn easily to liquid form. This supportive feature of the retina may lose in this transition which can cause to start detaching from the retina. When detaching it pulls retina and leads retinal tears. Liquid-form vitreous get into this torn tissue and lead retinal detachment.
Retina has a contact with vitreous gel inside of the eye. Vitreous gel is homogeny, tight, support the retina and pushes outer tissues such as choroids and sclera in healthy eye. Vitreous gel’s viscose and homogeny structure may change in some special cases. High myopia, eye trauma and intraocular inflammation diseases may vitreous gel turn easily to liquid form. This supportive feature of the retina may lose in this transition which can cause to start detaching from the retina. When detaching it pulls retina and leads retinal tears. Liquid-form vitreous get into this torn tissue and lead retinal detachment.
WHY RETİNAL DETACHMENT İS DANGEROUS AND URGENT?
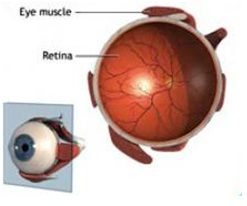 Retinal Detachment might lead to blindness. Cells will not be able to nourish itself and die because, the retina detached from the layer to which is attached. If retinal detachment moves to macula, it might cause vision loss. Even it is replaced perfectly with operation, cells might die due to the elapsed time, and it becomes impossible to have previous vision in the most successful sugeries.
Retinal Detachment might lead to blindness. Cells will not be able to nourish itself and die because, the retina detached from the layer to which is attached. If retinal detachment moves to macula, it might cause vision loss. Even it is replaced perfectly with operation, cells might die due to the elapsed time, and it becomes impossible to have previous vision in the most successful sugeries.
RETINAL DETACHMENT FACTS THAT NEED TREATMENT
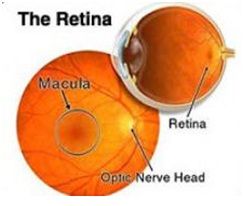
In Patients who have;
- Retinal detachment in the other eye.
- Other retinal detachment disease in family.
- Family history of retinal detachment.
- Retinal tears
- Plans for the eye surgery.
- Work that have high risk of head or eye trauma.
RETINAL DETACHMENT
 Retinal detachment is observed 1 person out of 10.000 every year. It is a big treat for vision. It is mostly seen at middle age, but it can be at any age. If it is not treated on time, it might cause complete vision lost or part of vision.
Retinal detachment is observed 1 person out of 10.000 every year. It is a big treat for vision. It is mostly seen at middle age, but it can be at any age. If it is not treated on time, it might cause complete vision lost or part of vision.
Retinal detachment is nerve layer separated from pigment epithelium layer so liquid weeps between those two layers because of tears or holes. Retinal detachment is mostly seen in high myopia patients. Retina layer became unshaped and thinner when eye’s front and back diameter increased. Due to ome other reasons retina can get thinner such as family and degenerative diseases. Vitreous gel started to lose homogeny and turn to liquid form. During this period, it starts to come off from retina and that is called Vitreous Retinal Detachment.
CAUSES AND SYMPTOMS OF RETINAL DETACHMENT
 Unshaped and thin retinal layer can cause jag on retina. This jag feels like lightning or flashing. Those flashes can take one day long or longer. Some of the patients do not even feel them. If there is a vein passing through this tear on retina, it might cause bleeding so patients will see like soot rain. Vitreous gel’s viscose and homogeny structure may change and turn easily to liquid form.
Unshaped and thin retinal layer can cause jag on retina. This jag feels like lightning or flashing. Those flashes can take one day long or longer. Some of the patients do not even feel them. If there is a vein passing through this tear on retina, it might cause bleeding so patients will see like soot rain. Vitreous gel’s viscose and homogeny structure may change and turn easily to liquid form.
Vitreous supportive feature is lost in transition to liquid form than it starts to split from retina. When it is splitting it pulls retina and retinal tears might occur. Vitreus gel starts leeking through this tear and cause retinal detachment. Retina loses function and patients feel black spot or curtain in front of their eyes.
Retinal detachment sometimes stays on the same spot but it usually moves around. Central vision is lost when macula separated from tissue and eyeball shrinks when retinal detachment takes long time. Sudden hits to eye might cause retinal detachment also diabetes and family history, degenerative diseases might cause retinal detachment without tear or hole on retina.
DIAGNOSE
Pupils enlarge with eye drop and doctor search for tear or hole in the eye with microscope. Ultrasonography can be done if it is needed.
THE FACTS OF RETINAL DETACHMENT
Retinal Detachment can cause blindness so the facts are important. The facts are;
- Flashes with your eyes oper or closed.
- Seeing flying substance in front of your eye
- Black-gray curtain in vision
- Blurry vision and lost vision that can not disappear with a blink.
Patients must go for retina exam if they have any of these facts as soon as possible.
TREATMENT OF RETINAL TEAR
Early diagnosis is very important for retinal tear before it turns to retinal detachment. Sudden flashes and flying substance in front of the eye are symptoms of retinal tear. Patients must go for retina exam if they have any of these symptoms as soon as possible. Doctor might find tear on the retina while examination and must treat with laser beam to seal the tear.
WHAT İS TREATMENT OF RETINAL DETACHMENT?
Surgery is needed if retinal detachment is grown. Operation method shows differences for shape of tear, size, place and duration.
SCLERAL BUCKLİNG TECHNİQUE:
This is the oldest method applied in retinal detachment surgery. Hard silicon piece is placed on the tear to push it back to the retina wall. After this procedure all the fluid which has accumulated is absorbed.
VİTRECTOMY:
If Retinal detachment has many tears, big tear or undetected place might need vitrectomy operation during which the doctor can easily interfere the detachment inside of the eye. Small holes thru which vitreus fluid is cleaned using with aspiration prob sticks and light sourses are made on the eyeball. The fluid under retina is absorbed and, tears are treated with laser beam. A tampon material which could be made of air, gas or silicon oil is placed to keep the tears closed. Patients must wear eye patch and sleep in specific position after the operation.
UVEİTİS
UVEİTİS?
 This is an inflammation of the layers of the eye. The jelly-like material in the center of ball-shaped eye is surrended by 3 different layers. The outer layer is Sklera, the inner layer is Retina which allows us to see and Uvea is in the middle. Uveitis is the inflammation of Uvea. There are many tiny vanes feeding our eye in the Uvea. But the inflammation also affects the other layers and tissues in the eye. This situation which requires an expert is uveitis may give a serious threat to our vision The treatment can only be successful provided that this disease is understood, accepted by the patient well and treated on time.
This is an inflammation of the layers of the eye. The jelly-like material in the center of ball-shaped eye is surrended by 3 different layers. The outer layer is Sklera, the inner layer is Retina which allows us to see and Uvea is in the middle. Uveitis is the inflammation of Uvea. There are many tiny vanes feeding our eye in the Uvea. But the inflammation also affects the other layers and tissues in the eye. This situation which requires an expert is uveitis may give a serious threat to our vision The treatment can only be successful provided that this disease is understood, accepted by the patient well and treated on time.
It may affect either the uvea only or all the layers (Choroid, Iris) at the same time. This is not same as other infectious inflammations. On the contrary, it may also have started by infectious then continues due to the changes in our immune system. This makes it very complicated and varied from one patient to the other. The treatment plan must be very personal as itself. The dosage of the medication in the treatment must be determined by only expertise’s in Uveitis.
CAUSES
 The reason cannot be diagnosed 30-40% of the uveitis patients. They could be viruses, fungal infections and parasites or any symptoms of other sickness appeared in the eye. Therefore, it may require different kind of examinations and tests to find it out. Some systematic diseases such as Behçet’s disease, rheumatoid arthritis or spondylitis achilleate may also cause this disease.
The reason cannot be diagnosed 30-40% of the uveitis patients. They could be viruses, fungal infections and parasites or any symptoms of other sickness appeared in the eye. Therefore, it may require different kind of examinations and tests to find it out. Some systematic diseases such as Behçet’s disease, rheumatoid arthritis or spondylitis achilleate may also cause this disease.
DISEASES WHICH MAY CAUSE UVEITIS
- Behçet’s disease
- Infections
- Tuberculosis, Herpes etc.
- Eye traumas or surgeries
- Immune System Disorders, Rheumatism, Ulser etc.
EARLY SYMPTOMS

- Sensitivity to the light,
- Blurry or cloudy vision,
- Redness in the eye,
- Severe pain in or around the eye,
- Floaters,
- Glares,
- Lacrimation.
DIAGNOSE
Uveitis is an emergency case at any level. When medical intervention is applied late, it may progress for worse and cause permanent diseases like dysmorphias on the iris, cataract or glaucoma. The first thing to do is to get examined by an expert as soon as possible. The later you may visit your doctor the worse the vision loss to be.
 In some cases, Uveitis can be diagnosed at first sight. Even in these cases, FFA or Ultrasonography is mandatory to find out any possible threat to the vision. Afterwards, Rheumatologists, experts in dermatology or chest diseases or neurologists may carry out some joint research.
In some cases, Uveitis can be diagnosed at first sight. Even in these cases, FFA or Ultrasonography is mandatory to find out any possible threat to the vision. Afterwards, Rheumatologists, experts in dermatology or chest diseases or neurologists may carry out some joint research.
TREATMENT
- Treatment of any possible causing disease
- Sunglasses may help
- Daily activities usually are not limited. But, if the vision is reduced by the sickness or drops that are used to enlarge iris, it is not recommended to drive or works which require utmost care.
- Diet: There is no specific diet unless steroid use is necessary for the treatment. If so, No-Salt Diet is applied.
- Eye Specialist’s treatment
- Medication: Eye drops, steroids or injections.
- Medication used to improve immune system.
- Treatment of the disease which may cause Uveitis can also be beneficial.
It is important to follow up the patients since, some significant symptoms can also be observed during the examination or follow-up. These diagnoses are vitally important to your treatment.
OCULAPLASTY
EYELİD ESTHETİCAL SURGERY
Some changes may occur on eyelids caused by aging such as eyelid bags, outgrowth skin and wrinkles at the outer corners of the eye as known as goose’s feet.
Patients have Blepharoplasty operation for those changes around their eyes.
SURGERY AND POST-OPERATİON
- SURGERY AND POST-OPERATİON
- Anesthesia: Usually local anesthesia,
- Duration: 45 minutes for 2 eyelids
- Eye do not need to be covered.
- Cold compress 1st 24 hours after operation. Eye lids will be swollen and purple.
- Stitches: Stay one week.
- Controls: Day after operation, 7 days later and 1 mount later.
- Eye drops and Pomades: 1-week antibiotic pomades with steroid, 1-week antibiotic eye drop.
EYELİD DROP (PTOSİS)
Upper eyelid drop is called Ptosis. It could be observed any age.
FACTS OF PTOSİS
- Neurogenic Facts: Nerves that hold the eyelid up may cause
- Myogenic Facts: Muscle problem on eyelid (it could be genetical)
- Senile Facts: Aging and eye surgery
- Mechanical Facts: Fact that make eyelid heavy (Eyelid tumors and Hematoma)
TREATMENT OF PTOSİS
Surgery is the treatment for Ptosis. There are two techniques for ptosis surgery:
- Elevator Resection: This can be used if the eyelid muscle functions strong enough.
- Frontalis Sling: This can be used if eyelid muscle does not function properly. It can be in patients who have congenital eyelid problems or nerves stroke on the eye and have had ptosis surgery before but didn’t benefit from. After surgery in rare cases, the eyelids may not fully close.
SURGERY AND POST-OPERATİON
- Anesthesia: Usually local anesthesia.
- Duration: 40 minutes for 2 eyelids
- The eyes must be covered with bandage.
- Eye lids will be swollen and purple.
- Stitches: Stay one week
- Controls: Day after operation, 7 days later and 1 mount later.
- Eye drops and Pomades: 1 week pomade with antibiotic and steroid, 1-week antibiotic eye drop.
FRONTALİS SLİNG
- Anesthesia: Local anesthesia for eyelids and forehead. General anesthesia for toddlers.
- Duration: 15 minutes per eyelid.
- The eye must be covered with bandage which will be taken off next day of surgery.
- Eye lids will be swollen and purple about one week.
- Stitches: Stay one week.
- Controls: Day after operation, 5 days later and 1 mount later.
- Eye drops and Pomades: 1 week pomade with antibiotic and steroid, 1-week antibiotic eye drop.
INTROVERTED EYELİD (ENTROPİON)
When eyelid turns inside it is called Entropion. It is usually observed on the lower eyelid. It is rarely seen on the upper eyelid. Entropion can be related to senile eyelid relaxation or congenital scars.
SYMPTOMS OF ENTROPİON
- Eyelid turns inside.
- Dilution, flagrancy and redness on the eye.
- Surgery is the treatment for Entropion. There are different techniques for Entropion surgery.
EVENTUAL PROBLEMS AFTER SURGERY
- Eyelid might turn inside again.
- If an excessive correction is made, then it may turn outside.
- Infection on the incision area.
SURGERY AND POST-OPERATİON
- Anesthesia: Usually local anesthesia.
- Duration: 40 minutes for 2 eyelids.
- Patients do not need to cover eye.
- Stitches: Stay one week
- Controls: Day after operation, 7 days later and 1 mount later.
- Eye drops and Pomades: 1 week pomade with antibiotic and cortisone, 1-week antibiotic eye drop.
RİTORNAL EYELİD (ECTROPİON)
When eyelid turns outside it is called Ectropion. It is observed on the lower eyelid. Ectropion can be related to senile eyelid relaxation or congenital scars. Also, it may relate to face nerve stroke and mass on lower eyelid.
SYMPTOMS OF ECTROPİON
- Eyelid turns outside.
- Dilution
- Dryness on the retina
Surgery is the treatment for Ectropion.
SURGERY AND POST-OPERATİON
- Anesthesia: Usually local anesthesia.
- Duration: 40 minutes for 2 eyelids
- Eyes do not need to be covered with bandage.
- Stitches: Stay one week.
- Controls: Day after operation, 7 days later and 1 mount later.
- Eye drops and Pomades: 1 week pomade with antibiotic and steroid, 1-week antibiotic eye drop.
CHALAZİON
There is fat layer under eyelid connected to eyelash root pores. Inflammation caused by make up, get fat on pores so fat layer under eyelid got swollen. It turns to mass later.
TREATMENT OF CHALAZİON
Antibiotic eye drop uses for avoids infection. Hot drains apply to inflamed eyelid to enlarge pores. If not treated on time it might turn to mass, it is need to clean with surgery.
CHALAZİON EXCİSİON
- Anesthesia: Usually, local anesthesia
- Duration: 10 minutes for 2 eyelids
- Eyes must be covered with bandage which will be taken off on the next day.
- Eye lids will be swollen and purple about one week.
- Controls: Day after operation and 1 mount later.
- Eye drops and Pomades: 1 week pomade and eye drop with antibiotic.
FAT PLAQUE ON EYELİD (XANTHELESMA)
Xanthelasma is fat-cholesterol plaque on eyelid. Usually observed on women and it is seen inside of both eyelids. Doctors are being suspicious about high cholesterol if patients are early age. Surgery is the treatment for Xanthelasma.
There will be no scar after the surgery.
SURGERY AND POST-OPERATİON
- Anesthesia: Usually local anesthesia.
- Duration: 10 minutes for 2 eyelids
- Eyes do not need to be covered.
- Eye lids will be lightly swollen and purple about one week.
- Stitches: Stay one week
- Controls: Day after operation, 7 days later and 1 mount later.
- Eye drops and Pomades: 1 week pomade with antibiotic.
EYELİD MASSES
There are Benign Mass and Malignant Mass.
BENİGN MASS
- Viral wart
- Dermoid cyst
- Seborrhoeic Keratosis
- Actinic Keratosis
- Cutaneous Horn
- Pyogenic Granulomatous
- Mole
- Keratoacanthoma
- Capillary Hemangioma
- Porto wine spot
MALİGNANT MASS
- Adenoid – Basal cell carcinoma
- Squamous cell carcinoma
- Sebaceous cell carcinoma
- Melanoma
- Merkel’s cell carcinoma
- After surgery those mass samples should send to pathology.
EYELASH TURN İNSİDE (TRİCHİASİS)
It can be seen on eyelid disease and long-term infection. Trichiasis is not good as esthetically also it feels sting in the eye. These lashes rub on the cornea and might damage it.
TREATMENT
Eyelashes that turned inside are removed with nipper. It is not permanent solution so eyelash will grow again within 3 mounts.
Eyelash that turns inside burned with cautery. It is permanent solution, but it might need few sessions.
Eyelash roots that turn inside froze with Kyro. It is permanent solution, but it might need few sessions.
LACMİRAL DUCT OCCLUSİON
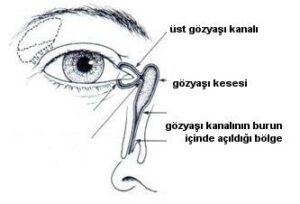 Liquid that humidifies eye flows through lacmiral duct to inside of nose. Usually, occlusion of lacmiral sac leads to Lacmiral Duct Occlusion disease. It is mostly seen in newborn babies, middle-aged woman and patients who have dysmorphias in the nose. When the lacmiral duct is blocked, liquid cannot flow to the nose so it will be leaking out from the eye. It causes infection on eye.
Liquid that humidifies eye flows through lacmiral duct to inside of nose. Usually, occlusion of lacmiral sac leads to Lacmiral Duct Occlusion disease. It is mostly seen in newborn babies, middle-aged woman and patients who have dysmorphias in the nose. When the lacmiral duct is blocked, liquid cannot flow to the nose so it will be leaking out from the eye. It causes infection on eye.
SYMPTOMS OF LACMİRAL DUCT OCCLUSİON
- Heavy dilution,
- Blurry eye
- Infection comes out from duck with pressing on nasal roots.
- Swelling of nasal roots
TREATMENT OF LACMİRAL DUCT OCCLUSİON ON BABİES
Massage technique applied to nasal roots in first year. It will apply 5 minutes each 3 o 4 times a day. Probability of success is around %95 in massage technique.
Antibiotic eye drop is used in patients who have blurry eyes.
If massage technique is not successful, doctors will use probing technique. Second probing will apply if the first one is not successful.
If Both probing is not successful, then patients wait until 3 years old and have dacryocystorhinostomy operation.
TREATMENT OF LACMİRAL DUCT OCCLUSİON ON ADULTS
1- MULTİDİODE LASER OPERATİON
Laminal Duct Occlusion is very quick and bloodless with Multidiode Laser operation.
WHAT ARE THE ADVANTAGES OF MULTİDİODE LASER OPERATİON BETWEEN OTHER SURGERİES?
- Most important advantage of multidiode laser is duration of surgery. It takes about 8 to 10 minutes.
- It slightly or never bleeds.
- Tissues may slightly be damaged.
- Recovery duration is very short. Patients can return their daily lives.
- There are no lacerations in this operation.
- Patients who have Lacmiral Duct Occlusion surgery before have more chance to have successful operation.
- Procedure can be watched with endoscope inside of the nose and the doctor interfere from here if it’s necessary.
WHAT İS THE DEPENDENCES SUCCESS ON SURGERY? CAN SURGERY REPRODUCE?
Success of surgery depends on the doctor’s experience. Patient should have good examination before the surgery. Success rate is around 90 % in this technique whereas the sucsess rate could only be around 87.5 % in the other surgeries. If another surgery is needed then success rate can be 100 %.
2-DACRYOCYSTORHİNOSTOMY (OPEN SURGERY)
Doctors apply laceration on nasal root about 1 cm under local or general anesthesia.
- A small window made on nasal bone.
- Doctors make straight entrance from lacmiral sac to nasal cavity.
- Silicon tubes can be used through punctum in some situation.
- Lacerations closed with stitches and surgery ends.
COMPLİCATİONS OF DACRYOCYSTORHİNOSTOMY OPERATİON.
- Infection on the area
- Recurrence
EYE PROSTHESİS
Usually, prosthesis is used in patients who have lost their eyes by accident or some other reason. This prosthesis does not provide vision but can make the eye ecstatically look good.
Doctors take out the eyes that lost vision, have bad appearance or steadily ache. There are different techniques for that operation.
- Taken out whole eyeball (Enucleation) It is used in case of eye tumors.
- Taken out inside of eyeball (Evisceration) It is used for other reasons than tumors. There are 2 kinds of prosheses which are internal prosthesis and external prosthesis.
Internal prostheses are made of special materials, and it is used after Evisceration operation to fill inside of eyeball. External prostheses are used after enucleation operation.
COMPLİCATİONS OF PROSTHESİS
- Itcy Eye and mucus-like liquid.
- Displace of the eye hole.
- Eyelid deformation
ADVİCES FOR PROSTHESİS USER
- Do not take off the prosthesis while sleeping to keep the shape still and the fluid less.
- Wash your eyelash roots with baby shampoo and rinse with warm water.
- Use artificial tear on prosthesis in daytime.
- Use glasses. It will protect healthy eye and prosthesis will not take attention.
STRABİSMUS
This is a critical situation which occurs due to the incoordination with the movements of the eyes or in the situation visual axes are not parallel to each other.
Strabismus is a disease that occurs in early ages and causes Amblyopia later. Strabismus can be treated both by surgical methods and non-surgical methods.
DRY EYE
DRY EYE
Usually our eye is lubricated and moisturized by the tear film. Tear film makes our eye comfortable and moisturizes but sometimes tear can be inefficient, or quality of tear might be very weak which leads Dry Eye. Tear is produced in two ways.one of which is continuous tear production and second one is overproduction of tear due to weeping, cold air or wind, foreign object damage and catching cold or flu may cause over lacrimation. It is interesting that dryness on the eye and contact lens usage can cause lacrimation too.
SYMPTOMS OF DRY EYE
- Burning or itchy feeling
- Have mucous ropes inside of the eye or around it.
- Redness,
- Heavy lacrimation and tiredness
- Uncomfortable feeling on contact lens usage
WHAT IS TEAR FILM LAYER?
When we blink, tear covers eyeball, and it makes layer on it. It is called Tear Film Layer. There is oil, mucous, electrolyte, vitamins, sugar and amino acid in Tear Film Layer. It nourishes front layer of the eye. It provides oxygen trespassing and protect from materials. It is impossible to have a clear vision without this layer. It contains immunoglobulin and immunomodulatory to protect the eye from microbial materials.
WHAT İS THE REASON OF DRY EYE?
Amount of tear decreases as we age. It is mostly seen in elder woman, but it can be seen at any age and gender. It may develop rarely due to the lackness of vitamin A in undeveloped countries. There might be other reasons too. If patient have articular pain beside dry eye, Sjögren Syndrome might be the reason. Some medicines reduce tear, and it might cause dry eye. These medicines are:
- Diuretical
- Beta Blockers
- Antihistaminics
If patients need to take this medication, they might use artificial tear drop. People who have dry eye are more able to get side effect for artificial tear drop with toxic. Some eye drops can contain protectable materials so it may irritate the eye.
HOW TO DİAGNOSİS DRY EYE?
Any ophthalmologists can diagnosis dry eye, but they must run tear calculation test for accurate result.
Schirmer Test: A filter tissue placed under eye lid, and it calculates if tear is enough or not. Tear should be less than 10 mm to be dry eye.
Tear film break-up time: Colorant drop under eye lid and blink couple times and wait 10 seconds without blink to see if there are any dry spots. It is important for diagnosis.
TREATMENT
1- TEAR ADDİNG
Artificial tear drops which are very similar to tears must replace the deficient amount of tear. They both moisturize the eye and keep wet. There are many kinds of artificial tear drop. Patients who use contact lens and are sensitive for preservative substance should use non-preservative eye drops. Artificial eye drops are used few times a day. Patient should follow doctor’s instruction.
2- PERMANENT AND TEMPORARY PUNCTUM(PLUG)
There is other way to keep the eyes moisturized and provide lacrimation. It is applied to keep the existing tear. Tears leak into the nose thru ducks in our nasal system. (When we cry our nose also leak.) We can block those ducks temporarily or permanently to keep tear and artificial tear in the eye long time.
3- OTHER TECHNİQUES
Tears also evaporate as same as other liquids. It can be useful to keep our home or room humid to prevent evaporation, so a cup of water placed on the top of stove or heater in winter. Person who has dry eye should protect their eyes from heat, steam also cigarettes smoke. Eye drops that contain vitamin A are useful for Stevens Johnson syndrome and pemphigoid.
CONTACT LENS
WHAT İS CONTACT LENS?
Contact lens is alternative solution for glasses which are used for refractive disorders. They are also used for cosmetic and treatment.
All principles of glasses are applied in contact lenses. Myopia and hyperopia can be corrected with contact lens that related to cornea shape and glass prescription. changed cornea shape cause astigmatism so patients must wear hard contact lens or special made (Toric) soft lens. The lens prescription must be same as glass prescription. Patient who has high myopia should use lower and hypermetropia should use higher prescriptions.
HARD LENS (GAS PERMEABLE)
It allows oxygen to go through to eye that is why it is called permeable hard lens. They are especially very suitable for keratoconus or astigmatism at high level.
SOFT LENS
There are many types of soft lens. Disposable lenses could be daily, monthly, 3 mounts, or 1 year wear or they could be bifocal or colored lenses. The usage of these lenses is very comfortable and worn for curative purposes too.
THE ADVANTAGES OF LENSES OVER GLASSES.
- Objects are seen in original size.
- Visual field of Lenses are larger than glasses. Side view of glasses is weaker.
- Contact lenses don’t have an edge whereas people with glasses always see the frame.
- There is no evaporation on contact lens.
- Contact lenses do not bother while doing any activities.
- Patients can easily wear sunglasses with their contact lenses on.
- Lenses are much lighter and more comfortable to use comparing to glass wear.
BEFORE YOU BUY CONTACT LENSES
Unsuitable Contact lenses may cause problem. Normal or Colored Contact lenses should be bought after full eye examination. Doctors should determine the most suitable power, radius and type of contact lens in the examination. Our center will give you trial lens if you have not experienced it before. When the proper use of lenses is understood well, our center then will give you real contact lenses, lens storage case, care solution and the manual.
THINGS TO REMEMBER
- You should wear contact lenses if your eye doctor determined.
- You should never keep wearing expired lenses even it feels alright.
- You should go to routine eye examination.
- Patient should clean, disinfect and rinse every time they take them out.
- Do not use the lens solution more than once. Refresh it before use.
- Do not share lens with someone else.
- Do not use any hair spray or perfumes after you have put them on.
- Do not put any make up inside of the eyelid and never use any eye drops unless it is prescribed by your eye specialist.
- Do not touch the top of solution bottle with your finger or contact lens.
- Do not continue using your contact lenses in case of any infection or discomfort in your eyes.
PRESBYOPİA
Presbyopia is a gradual loss of focusing ability of the lens on near objects. Because of some changes in our eye muscles, the shape of the lens is also affected. Presbyopia starts at the mid 40’s and finally affects everyone.
The main problem is very similar to hypermetropia. Focal point of light rays coming from near objects remains behind the retina and out of focus. In Hypermetropia, eyeball is shorter than a normal one. But In Presbyopia, that aged lens become harder and less flexible. This change causes difficulty in accurate refraction of the light rays to focus in front of the retina.
Reading may be more difficult at night or in dim light when you are tired. Presbyopia occurs regardless of your refractive disorder.
The first symptom of Presbyopia is feeling necessity to keep the near objects away from you while you are reading. As the time passes blurry vision increases and pain occurs at forehead and temple. Focusing the eye on near objects by force cause other problems. After reading, clear vision for distant objects might temporarily be difficult due to the ability of focusing. The only solution of Presbyopia is optical correction (reading glasses or contact lenses). For myopia, people using corrective lenses may need bifocal glasses (upper part is used for distant vision and the bottom part is for near vision) or they use two separate glasses for different distances.
Because Presbyopia progress until the age of 60’s prescriptions change frequently. After 60’s, presbyopia becomes more stable. From the age of 60-65 focusing ability of the eye stops since the lens has lost its flexibility; at this level near vision is completely dependent to the glasses. However, Myopia people sometimes take off their distant glasses for near vision and they can do their activities more comfortably.
THE SYMPTOMS OF PRESBYOPIA
Patients with presbyopia find difficult to see the objects near than 50 cm. For this reason, they can have a better vision by moving the objects away. As time passes if the patient has poor near vision, they also may have some pain in the forehead and temple.
TREATMENT
There are many kinds of treatment methods in the world. These treatment methods have their own advantages and disadvantages. Today we treat presbyopia in our hospital either multifocal lens implementation or presyllabic laser which has been known as the most reliable method in the whole world for the Presbyopia.
- TREATMENT WITH GLASSES
- Bifocal Glasses
- Multifocal (progressive) glasses
- TREATMENT WITH CONTACT LENSES
- Multifocal contact lenses: Patients who are found suitable for lens use. However, patients over 40 years of age may face some difficulties in use due to the poor tear quality. Monovision with contact lens (leaving one eye myopia): Adaptability to the treatment becomes certain only after the first examination.
- SURGICAL TREATMENT
- There are 2 different places for this treatment.
- CORNEA
- Presbylasik Treatment
- Monovision excimer laser treatment
- LENS
- Multfocal Lenses
- Accommodative Lenses
CORNEAL TRANSPLANTATİON
CORNEAL TRANSPLANTATİON (KERATOPLASTY)
Keratoplasty is an operation in which the foremost transparent layer that is defected for some reason is changed with a healthy corneal tissue derived from a donor.
A circular tissue in 6-9 mm is taken out from the healthy cornea of the donor and replaced with the patient’s damaged cornea in surgery.
With the developing technology, corneal transplants may be performed by Intralayer Laser technology. In this operation, the damaged layer of the cornea is cut with laser beam which does not cause any deformation on the healthy side of the eye. The same technique is applied on the healthy corneal layer according to the need of the patient’s eye. Corneal transplantation is always performed under general anesthesia. The biggest advantages of IntraLase are having almost no risk of tissue rejection in separation of the damaged and healthy tissue.
Patients should be very carefull about hygiene and avoid rubbing their eyes firmly and protected it from any traumas such as bumping or hitting.
In case of any pain, redness, blurry vision, sensitivity to light after the operation, they should consult their doctor. These symptoms maybe the symptoms of red reaction and it needs urgent treatment.
The patients should have a good relationship with the doctor. It is not satisfactory to have a successful operation without routine eye exams especially within 1 or 2 years after the operation.
FACT CAUSE KERATOPLASTY

- Corneal Dystrophy is genetic (known as spotting eye ),
- Keratoconus (Chronic deformation of Cornea),
- Cornea injuries,
- Corneal infection,
- After chemical injuries,
After the corneal transplantation the success and the best vision depends on the strength and healthy tissues including all the veins and nerves behind the eye.
NEURO OPHTALMOLOGY
WHAT İS NEURO-OPHTALMOLOGY?
It is a discipline dealing with common diseases of the eye and the nerve system. Our vision is comprised of perception of the eye firstly and perception of visual center located in the back of the brain. Visual pathways from optic nerve, an eye nerve, to the visual cortex in the brain where our vision is formed, or the diseases occurred in the cortex could be the subject of Neuro-ophthalmology. Also, it deals with the movements of both eyes accordingly. The reasons and distinguishing diagnosis of the headache caused by eye disorders are in the scope of the Neuro-ophthalmology. It contains temporarily vision loss, double vision and the pupils in different size.
NEURO-OPHTALMOLOGY DEALS WITH
- Different size eye pupils,
- Eye complaints related to Multiple sclerosis (MS),
- Eye complaints related to Myasthenia gravis,
- Color vision defects,
- A region that cannot be seen in the visual field,
- Double vision,
- Thyroid-related eye disease,
- Sudden loss of vision,
- Slowly progressing vision loss,
- Fleeting loss of vision,
- Migraine and migraine related eye pains,
- Eye complaints related to strokes,
- Facial palsy and facial spasms.
SYMPTOMS AND CAUSES
- Temporarily loss of vision: blackout in one or two eyes or temporary vision loss may be the symptom of temporary conjunction of the veins going to the eye or the visual center in the brain. It should be evaluated immediately. It may be related to problems of heart valves of the young or problems of cardiovascular and jugular vein in the neck of old people. If not treated it may cause embolism and finally permanent loss in vision.
- Sudden loss of vision: it has a medical emergency. It may be a symptom of obstruction in blood vessels going to eye or visual center in the brain. It is necessary that a doctor should see it within a few hours. Sometimes it may not relate to vessels, but to diseases causing conjunction in the optic nerve.
- Slowly progressing vision loss: Generally, slowly progressing vision loss can occur due to some diseases like cataract, glaucoma, yellow dots or any vitally important reason that press on the optic nerve.
- Double vision: In case there is unbalanced working of muscles that move the eye due to a problem of muscles or nerves moving the muscles, eyes would not be in parallel position and when two eyes send different messages to the brain, double vision arises. Ophthalmologist should control it as soon as possible and should find its reason. If problems at the nerves originate from the brain, neurological diseases should be searched and it should be cured. If it is related with the vessels, again the reasons at heart or situation at the brain are checked aand they should be treated. Treatment should be planned with neurology doctors if it is related with muscle disease affecting other muscles of the body and with endocrine surgeons if there is a problem at eye muscle related with hormonal disorders.
- Opening or decrease of the eyelid: In case there is an unbalanced operation of muscles that moves the eye due to a problem of nerves and muscles operating the eyelids, one or both eyelids may open or decrease. Opening is seen frequently on goiter disease, while the decrease is caused by expansion of brain vessels or muscle diseases. Since expansion of brain vessels is a life-threatening case, ophthalmologist should be consulted immediately if eyelids are decreased especially if pupils are grown.
- Pupil inequality: Size difference between the eye pupils is a natural case. If this difference is very big, or the difference becomes greater in the light or darkness, it may be a sign that there is an important problem at brain or neck vessel or an important lung disease. Without losing any time, getting in contact with an Ophthalmologist might save a life.
- Accident and impacts: Muscles or nerves of the eyelids may hurt visual nerve with eye muscles themselves or eye nerves. For the accidents and impacts that does not give any symptom at early period, an early symptom or treatment can be provided only after the careful examining of the ophthalmologist.
LACMİRAL DUCT OCCLUSİON
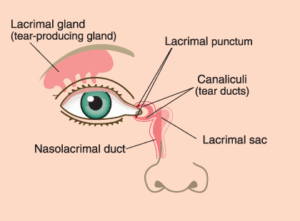
Liquid that humidifies eye flows through lacmiral duct to inside of nose. Usually, occlusion of lacmiral sac leads to Lacmiral Duct Occlusion disease. It is mostly seen in newborn babies, middle-aged woman and patients who have dysmorphosis in the nose. When the lacmiral duct is blocked, liquid cannot flow to the nose so it will be leaking out from the eye. It causes infection on eye.
SYMPTOMS OF LACMİRAL DUCT OCCLUSİON
- Heavy dilution
- Blurry eye
- Infection comes out from duck with pressing on nasal roots.
- Swelling of nasal roots
TREATMENT OF LACMİRAL DUCT OCCLUSİON ON BABİES
- Massage technique applied to nasal roots in first year. It will apply 5 minutes each 3 o 4 times a day. Probability of success is around %95 in massage technique.
- Antibiotic eye drop is used in patients who have blurry eyes.
- If massage technique is not successful, doctors will use probing technique. Second probing will apply if the first one is not successful.
- If Both probing is not successful, then patients wait until 3 years old and have dacryocystorhinostomy operation.
TREATMENT OF LACMİRAL DUCT OCCLUSİON ON ADULTS
- MULTİDİODE LASER OPERATİON
Lacmiral Duct Occlusion is very quick and bloodless with Multiride Laser operation.
WHAT ARE THE ADVANTAGES OF MULTİDİODE LASER OPERATİON BETWEEN OTHER SURGERİES?
- Most important advantage of multidiode laser is duration of surgery. It takes about 8 to 10 minutes.
- It slightly or never bleeds.
- Tissues may slightly be damaged.
- Recovery duration is very short. Patients can return their daily lives.
- There are no lacerations in this operation.
- Patients who have Lacmiral Duct Occlusion surgery before have more chance to have successful operation.
- Procedure can be watched with endoscope inside of the nose and the doctor interfere from here if it’s necessary.
WHAT İS THE DEPENDENCES SUCCESS ON SURGERY? CAN SURGERY REPRODUCE?
Success of surgery depends on the doctor’s experience. Patient should have good examination before the surgery. Success rate is around 90 % in this technique whereas the sucsess rate could only be around 87.5 % in the other surgeries. If another surgery is needed then success rate can be 100 %.
- DACRYOCYSTORHİNOSTOMY (OPEN SURGERY))
Doctors apply laceration on nasal root about 1 cm under local or general anesthesia.
- A small window made on nasal bone,
- Doctors make straight entrance from lacmiral sac to nasal cavity,
- Silicon tubes can be used through punctum in some situation,
- Lacerations closed with stitches and surgery ends.
COMPLİCATİONS OF DACRYOCYSTORHİNOSTOMY OPERATİON.
- Infection on the area
- Recurrence
MACULAR DEGENERATİON
Smoking, Genetic disposition or unhealthy nutrition are also risk facts of macular degeneration.
Macula is the center of the retina. The nerve roots behind the eye and the point in the retina provides most of the vision. Macula helps us drive, read or write with a clear vision which might not be possible in case of any damages on it.
The symptoms may vary from one patient to the other. Therefore, it could be hard to diagnose in the beginning. When it occurs in only one eye which most of the time is difficult to make sure that its only one eye, the other healthy eye can function for a long time. Whereas the central vision loss might be diagnosed earlier and easier.
Observing any distortions or blurriness in an article or a black point in the central of the vision are the first symptoms of the macular degeneration.

TYPES OF MACULAR DEGENERATİON
Dry Type: Dry AMD is an early stage of the disease and may result from the aging and thinning of macular tissues, depositing of pigment in the macula. It causes long-lasting visual loss and progress very slowly.
Wet Type: In this type, new sick blood vessels occur and progress to the macula. This can cause sudden vision loss which is observed more rarely than the dry type.
PEOPLE AT RİSK
One third of the People over 60 who have relatives having macular degeneration is more likely to have the risk. Women are more at risk rather than men. Also, people with diabetes, hypertension, color eyes, coroner disease, vitamin deficiency or smoking habits are in this group.
BLEPHARİTİS
This is a common inflammation of the eye lids with dry eye or bacterial infections. Some kind of skin conditions may also cause inflammation of the eyelids. It occurs where the eyelashes are.
SYMPTOMS
- Watery or red eyes
- A gritty, burning sensation in the eye.
- Eyelids that appear greasy, swollen or itchy
- Skin Flakes around the eyes
- Crusted eyelashes upon awakening.
- Eyelid sticking
- More frequent blinking
- Sensitivity to light
- Eyelashes that grow abnormally (misdirected eyelashes)
- Loss of eyelashes
DIAGNOSE
Eyelid examinations or swabbing skin tests help diagnose the disease. It can be diagnosed in a normal or regular eye exam since the inflammation can be seen very clearly.
TREATMENT
- Cleaning the affected area: It is very necessary to keep the affected area by cleaning regularly with a warm cloth.
- Medications: In case of bacterial inflammation, Eyedrops containing antibiotics help control the disease.
- Steroids or ointments. Eyedrops or ointments containing steroids can help control inflammation in your eyes and your eyelids.
- Artificial tears. Lubricating eyedrops or artificial tears are also very usefull for the blepharitis.
- Treating underlying conditions. Blepharitis caused by seborrheic dermatitis, rosacea or other diseases may be controlled by treating the underlying disease.
Unfortunatelly, it can relapse quite often althouh treated well.
CONJUNKTİVİTİS
This disease which is known as “Pink Eye” occurs due to an inflammation or infection of the transparent membrane (conjunctiva) that lines your eyelid and covers the white part of your eyeball. Inflammation of the tiny blood vessels in the conjunctiva makes them more visible which also makes eyes seen reddish or pink.
Bacterial or viral infection, an allergic reaction, or though pink eye can be irritating, it rarely affects your vision. Treatments can help ease the discomfort of pink eye. Because pink eye can be contagious, early diagnosis and treatment can help limit its spread.

COLOR BLİNDNESS (DALTONİSM)
Color blindness does not mean visual loss or full blindness. Deficiency in the way we see color can cause this problem in our vision. Some certain colors cannot be distinguished properly such as blue and yellow or red and green.
 This disease is mostly inherited and affects males more frequently than females. Red-green color deficiency is the most common form of color blindness. It might also occur due to the damages on our optic nerve or presence of Glaucoma.
This disease is mostly inherited and affects males more frequently than females. Red-green color deficiency is the most common form of color blindness. It might also occur due to the damages on our optic nerve or presence of Glaucoma.
SYMPTOMS
Difficulty in distinguishing those colors is the main sign of color blindness.
TREATMENT
Some time ago, it was not possible to treat the inherited color blindness but only the color blindness which gained after birth. But today, both types can be treated by the implementation of intraocular lenses in the eye.
AMBLYOPİA
If an eye cannot carry out proper visual acuity, it must be due to the amblyopia or with its common name “Lazy Eye”. It might be inherited infancy disease which require an urgent exam and treatment in children. Since those children are at the risk, their prompt eye check must not be ignored.
REASONS OF AMBLYOPIA
STRABISMUS: The most common reason of this disease is strabismus. It usually affects only one eye. If one of the eye fails to see properly, the healthy eye will be pushed to see automatically. In some cases, children may have misaligned or crossed eyes that are known as “Strabismus.”
REFRACTIVE ERRORS: If one of the eye has some blurry vision which might have occurred due to some refractive disorders, this eye means to have completed its development. This type of Amblyopia is the most difficult one to discern because of not having any visible sign. It can be treated upon to the recognition of any misalignment in the eye but then it is always too late. Therefore, all the children with or without any complaints must be examined to avoid any risk of Amblyopia under the age of 4.
Cataract can be another reason in infants. This is also very easy to be diagnosed with a basic examination. As the pediatrician observes cataract in the pediatric exam, the baby must go under surgery as it will cause Amblyopia very quickly.
DIAGNOSE
It can be very difficult to diagnose any sign of Amblyopia in children between 3,5 and 4 years old. The pediatrician manually examines each eye with the other eye closed. Each eye’s reaction is evaluated by the physician in order to find out Amblyopia. Also, each eye is examined just after the pupil has enlarged and its refractive ability is evaluated. Each eye also examined closely to seek any sign of misalignment or disorder. The most important point in the exam is to check if one eye has extremely more refractive error than the other eye.
TREATMENT
The most common way of treatment is to force the child to use the affected eye by patching the healthy eye for a long time. This is a long and annoying treatment for the child, so they attempt to take the patch off many times without our notice. İt is also necessary to patch the eye before medical intervention. During this period, parents should be very patient, tolerant and supportive by explaining the importance of patching.
CORNEA
The cornea is the transparent, dome-shaped window covering the front of the eye. It is also protective membrane for the retina. There is no blood vessel which makes the cornea transparent and shiny. It is nourished by the nerve endings in the Limbus.
LAYERS OF CORNEA
- Epithelium is the outer layer of the cornea, and it always regenerates if there is any injuries on the cornea
- Bowman’s Layer is just beneath the Epithelium. Since this membrane is very tough and hard to penetrate, it protects the cornea from any injuries.
- Stroma which gives the cornea its shiny appearance is the thickest layer, located in the center of the layers.
- Descemet’s Layer which pumps water into the eye is located between the Stroma and the Endothelium.
- Endothelium is the inner layer of the cornea.
Our eye should always be wet and nourished. The tear films keep the Epithelium wet meanwhile Aqueous keeps the Endothelium wet.